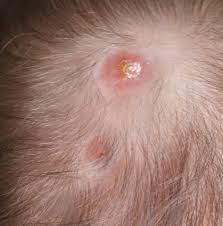
Acanthosis bullosa is a synonym of epidermolysis bullosa (EB). It encompasses a collection of rare conditions characterized by the skin’s heightened susceptibility to blistering. The fragility of the skin in individuals with epidermolysis bullosa becomes evident right from birth, making it susceptible to triggers like gentle touches, changes in temperature, or routine activities such as diaper changes.These triggers often lead to the development of painful blisters and wounds that exhibit slow healing.
The impact of EB on a child’s life varies significantly, ranging from mild cases that require precautionary measures to severe instances demanding ongoing medical attention.
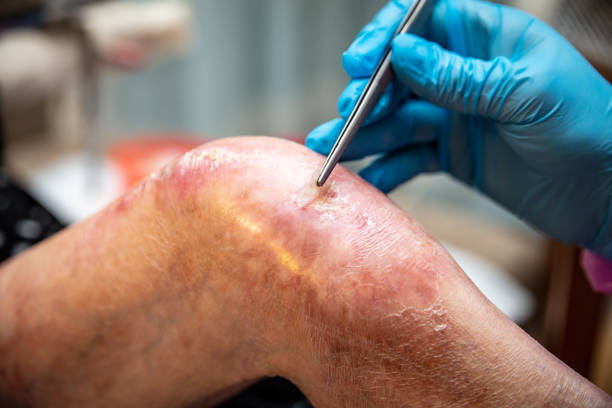
Types of Acanthosis Bullosa
The types of EB further highlight the diversity in symptoms.
Epidermolysis Bullosa Simplex (EBS):
- The most prevalent type.
- Manifests as blisters on newborns’ hands and feet, with possible thickened skin in adolescence.
- Severity varies, with widespread blistering potentially diminishing with age.
Dystrophic Epidermolysis Bullosa (DEB):
- Mild cases result in blisters on hands, feet, knees, and elbows.
- Severe cases lead to extensive blistering, missing skin, and potential need for a feeding tube.
- Scarring occurs during healing, affecting mobility.
Junctional Epidermolysis Bullosa (JEB):
- Mild cases show blisters on specific body parts in newborns, diminishing by a few months.
- Severe cases feature widespread blistering, affecting body organs and potentially leading to infections or breathing issues.
- Scarring may cause digits to join, but precautions can reduce risks.
Kindler Syndrome:
- Extremely rare form with sun-sensitive blistering in infancy, evolving into dark patches on the skin.
- Skin thins and wrinkles with age, resembling elderly hands and feet.
Epidermolysis Bullosa Acquisita (EBA):
- Uncommon autoimmune subtype beginning in adulthood, targeting collagen in the skin.
- Blisters may develop on hands, knees, and inside the body.
- Healing results in scarring and milia formation.
Despite the incurable nature of EB, ongoing research has led to improved understanding and treatments. Symptoms usually emerge at birth, but even milder cases might become noticeable when a child starts crawling or walking.
Symptoms of Acanthosis Bullosa

In most cases of Epidermolysis Bullosa (EB), symptoms become apparent either at birth or shortly thereafter. However, in milder cases, signs may only become noticeable when the child begins to crawl or walk.
Regardless of the onset, common manifestations include:
- Blisters and Wounds:
- The sensitive skin is susceptible to rapidly developing painful blisters, frequently triggered by gentle touches or sudden changes in temperature.
- The fragile nature of the skin earns children with EB the nickname “butterfly children,” likening their skin to the delicacy of butterfly wings.
- Wounds from ruptured blisters heal slowly, and some may persist for months or even years.
- Pain:
- Pain is a prevalent symptom, especially for those with severe EB.
- Causes of pain include blistering, raw skin, infections, bathing, bandage changes, and dehydrated skin.
- Pain management may involve regular use of medications, particularly during bandage changes.
Complications:
The condition can lead to various health issues or complications, such as:
- Anemia due to blood loss from wounds, impeding skin healing.
- Constipation, resulting from painful bowel movements caused by blisters in the rectal area.
- Dehydration from large, open wounds.
- Eye problems like pink eye, swollen eyelids, and impaired vision.
- Loss of flexibility in fingers or toes due to cycles of blistering and scarring.
- Hair loss if scarring occurs repeatedly on the scalp.
- Hardening and shortening of muscles, tendons, and tissues, causing pain and potential deformities.
- Infections due to open wounds, with symptoms like redness, pain, and fluid leakage.
- Intense itching caused by inflamed skin, overheating, dryness, and healing wounds.
- Malnutrition, often from the body using nutrients to repair the skin or due to painful blisters in the mouth or esophagus.
- Mobility problems due to blisters, pain, and scarring.
- Mouth-related issues like sores, cavities, and limited mouth opening.
- Nail loss or deformed nails.
- Narrowing of the esophagus or other areas due to internal scar tissue.
- Unpleasant odor from damaged skin, especially if infections are present.
- Diminished quality of life for both parents and children, impacting education, career, and emotional well-being.
- Increased risk of skin cancer, especially squamous cell carcinoma, in severe cases.
- Tiny white bumps called milia may appear when blisters subside.
Understanding the varied complications associated with EB underscores the importance of early detection and comprehensive care to improve the overall well-being of individuals affected by this condition
Who is Affected by Acanthosis Bullosa/Epidermolysis Bullosa (EB)?
Epidermolysis Bullosa (EB) is a rare condition, with an estimated 25,000 to 50,000 individuals affected in the United States.
Onset and Risk Factors:
- Most types of EB manifest in childhood, with fragile skin and blistering noticeable either at birth or shortly afterward.
- Mild cases may show signs when a child begins to crawl.
- Epidermolysis bullosa acquisita (EBA) is the only type that begins in adults.
- Children have a higher risk of developing EB if one or both parents carry genes for the condition.
- EB affects children of all races and ethnic groups.
Causes of Acanthosis Bullosa
- EB is not contagious; gene mutations cause all types except for EBA.
- Gene mutations result in a modified version of a gene, leading to a lack of proteins essential for holding the skin layers together.
- The absence of these proteins makes the skin extremely fragile, causing layers to slide against each other with minimal friction, leading to blister formation.
- The type of EB determines how easily the skin blisters.
- In EBA, considered an autoimmune disease, the body’s immune system mistakenly attacks and destroys the proteins responsible for holding skin layers together.
Tests, Diagnosis, and Treatment of Acanthosis Bullosa
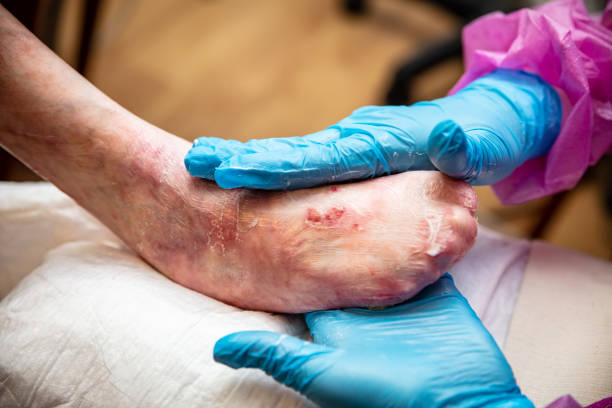
Genetic Counseling and Testing:
- Genetic counseling is essential for individuals with EB or a family history of the condition.
- Genetic testing helps assess the likelihood of having a baby with EB and is recommended before attempting to conceive.
- Identifying EB genes through testing can be a crucial step in making informed family planning decisions.
Prenatal Testing:
- It is possible to determine if a developing baby has EB through prenatal testing, although this poses risks to the baby and requires careful consideration.
Diagnosis:
- EB signs, like blistering or missing skin, are often evident at birth.
- Dermatologist or pediatric dermatologist consultation is crucial to identify the cause, ruling out conditions other than EB.
- Detailed examination of the skin and affected areas, along with family history questions, aids in diagnosis.
- Skin biopsy and genetic testing are commonly employed for accurate diagnosis and determining the EB type.
Treatment of Acanthosis Bullosa
- No cure for EB exists; lifelong care is typically required.
- Referral to specialized EB treatment centers is recommended for comprehensive care.
- Treatment involves wound care, pain management, injury prevention, and addressing complications.
- EB treatment centers offer multidisciplinary expertise, including pediatricians, dermatologists, nurses, dieticians, and psychologists.
- Care intensity varies; parents of children with mild EB may manage independently, while severe cases necessitate professional medical help.
Wound Care:
- Involves daily bandage changes, potentially requiring hours of attention.
- Severe cases may require nurse assistance for wound care at home.
Pain Management:
- Medications like antidepressants, antiepileptic drugs, acetaminophen, and opioids are used to alleviate pain.
- Pain management is essential for various activities, including bathing, wound care, and daily movements.
Preventing New Injuries:
- Padded bandages and loose-fitting clothes help prevent additional wounds.
- Detailed advice from dermatologists aids in injury prevention.
Complication Monitoring and Treatment:
- Regular monitoring for complications like anemia, cavities, constipation, and infections.
- Treatment involves iron supplements, dental care, diet modification, and antibiotics.
Other Complications and Treatments:
- Surgical interventions for fused fingers or toes.
- Fluid replacement for dehydration.
- Moisturizer application for dry skin.
- Treatments for excess sweating and eye problems.
- Intervention for complications like malnutrition, non-healing wounds, scarring, and mobility issues.

Living with Epidermolysis Bullosa (EB) and Supportive Measures:
Daily Challenges:
- Individuals with EB, often referred to as “butterfly children,” navigate daily challenges due to their fragile skin.
- Slow-healing wounds and the constant risk of blisters impact their routine activities.
Quality of Life Considerations:
- Coping mechanisms, emotional support, and financial considerations are essential for both parents and individuals with EB.
- The toll on education, employment, and daily activities can be significant.
Educational and Occupational Challenges:
- Children with EB may face difficulties in school due to health-related absences or physical limitations.
- As they grow older, pursuing employment or driving may pose challenges, requiring adaptability and understanding.
Support Systems:
- Emotional and psychological support for both individuals and their families is crucial.
- Support groups, counseling, and community networks can provide valuable assistance.
Skin Cancer Awareness and Prevention:
- Regular monitoring for skin cancer, especially squamous cell carcinoma, is vital.
- Preventive measures, such as avoiding sun exposure and prompt treatment of suspicious lesions, are emphasized.
NOTE: Dermatologists are dedicated to enhancing the quality of life for children coping with epidermolysis Bullosa (EB) and supporting their parents. They empower parents by providing crucial information for the care of their child, offering valuable tips to minimize discomfort.
Tips for Reducing Blisters:
- Opt for disposable diapers with Velcro fasteners instead of tapes to prevent them from sticking to the child’s skin.
- Protect the fragile diaper area by lining disposable diapers with a silicone contact sheet, available at medical supply companies.
- Dress your baby in a front-fastening, one-piece lightweight garment for easier dressing and undressing.
- Turn clothing inside-out to avoid seams rubbing against the skin, potentially causing blisters.
- Consider using therapeutic clothing tested in clinical trials, proven to be less irritating than regular clothing.
Preventing Glove-Related Injuries:
- During wound care, consider avoiding gloves and frequently wash your hands instead.
- If gloves are necessary, apply a friction-reducing ointment like pure petroleum jelly to minimize potential skin irritation.
Choosing the Right Skincare Products:
- Consult your child’s dermatologist if a skincare product becomes less effective, or if your child needs an anti-itch solution.
- Report complications promptly, such as blisters or scars, as early intervention can prevent further issues.
Encouraging Play and Movement:
- Despite fragile skin, encourage your child to play and move to prevent constipation and muscle-related complications.
Regular Full-Body Skin Exams:
- Schedule full-body skin exams starting at age 10, regardless of the EB type, to detect and address recurring wounds or persistent issues promptly.
These proactive measures can significantly reduce complications associated with EB, fostering a better quality of life for affected children. Regular skin exams are crucial for early detection, especially given the heightened risk of skin cancer in children with EB. Stay vigilant and report any concerns to your child’s dermatologist promptly.
Ongoing Research and Future Prospects:
Research Progress:
- While current treatments focus on symptom management, ongoing research offers hope for more effective therapies and potentially a cure.
- Advances in understanding the genetic and molecular aspects of EB are paving the way for targeted interventions.
Clinical Trials and Experimental Treatments:
- Participation in clinical trials and experimental treatments is an option for individuals seeking innovative approaches.
- Collaboration between researchers, medical professionals, and the EB community